That sudden, throbbing pain in your tooth can be alarming, bringing a wave of anxiety with it. You’re left wondering what’s causing such intense discomfort, whether it’s a true dental emergency, and what treatment might involve. More often than not, the source of this severe toothache is a common condition called pulpitis, which is an inflammation of the sensitive pulp tissue deep inside your tooth.
Feeling worried is completely understandable, but you don’t have to face this uncertainty alone. This reassuring guide is here to provide the calm, clear answers you need. We will explain the two different types of pulpitis, help you recognise the specific symptoms for each, and clarify when you need to see an endodontic endodontist immediately. Our goal is to empower you with knowledge, ease your concerns, and guide you towards the right steps for fast, effective relief.
Table of Contents
Toggle- First, What Is the Dental Pulp Inside Your Tooth?
- The Two Stages of Pulpitis: Reversible vs. Irreversible
- What Causes Pulpitis? From Decay to Dental Trauma
- Recognising the Symptoms: Is Your Toothache an Emergency?
- How a expert Treats Pulpitis to Relieve Your Pain
- Find Calm and Lasting Relief from Pulpitis
- Frequently Asked Questions About Pulpitis
First, What Is the Dental Pulp Inside Your Tooth?
If you’re dealing with a severe toothache, understanding the root of the problem is the very first step towards finding lasting relief. We know how distressing tooth pain can be, and our goal is to provide clear, reassuring information to help you feel in control. The pain you’re feeling often starts deep inside your tooth, in a place called the dental pulp.
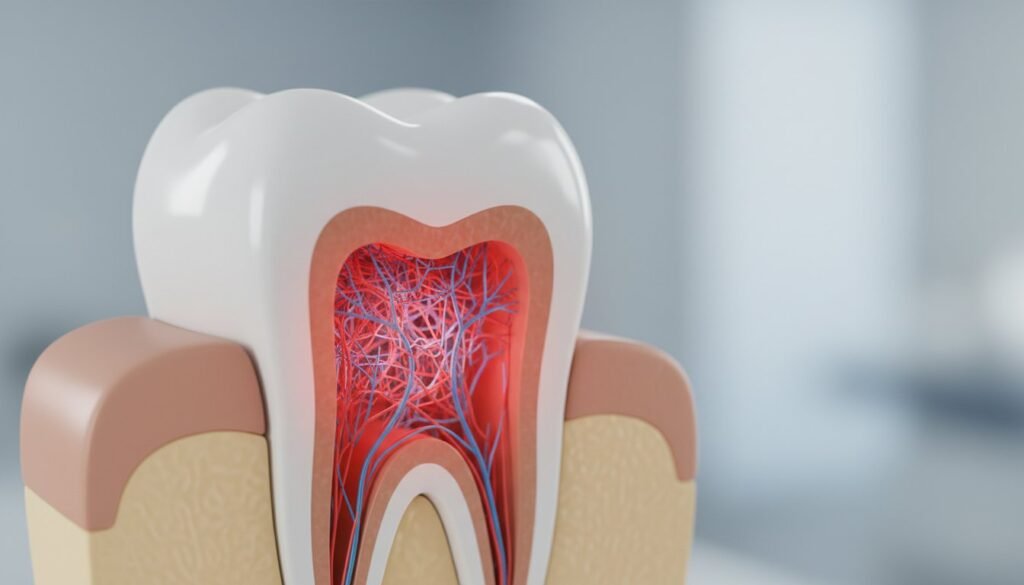
To picture it, think of your tooth as having three distinct layers:
- Enamel: The tough, white outer shell that protects your tooth from daily wear.
- Dentin: A softer, yellowish layer beneath the enamel that contains microscopic tubules leading to the tooth’s centre.
- Dental Pulp: The innermost chamber. This is the living, beating heart of your tooth, a soft tissue composed of nerves, blood vessels, and connective tissue.
This pulp is what keeps your tooth alive, healthy, and responsive. It’s a vital component that is normally well-protected by the outer layers of enamel and dentin.
The Role of the Pulp: More Than Just a Nerve
While many people refer to the pulp as simply “the nerve,” its function is far more sophisticated. The blood vessels within the pulp act as a lifeline, delivering the oxygen and nutrients needed to keep the surrounding tooth tissue healthy and strong. At the same time, the nerves provide sensory information, allowing you to feel temperature changes from hot tea or cold ice cream. This sensitivity is your tooth’s built-in alarm system, designed to alert you to potential harm and protect you from damage.
What Happens When the Pulp Gets Inflamed?
When bacteria from deep decay or trauma reaches this delicate inner tissue, it can become irritated and inflamed. This condition is known as pulpitis. To understand the specifics of what is pulpitis, it’s crucial to consider the tooth’s unique structure. Unlike inflammation in your skin where swelling can expand outwards, the pulp is encased within the rigid, unyielding walls of the tooth. As the pulp swells, intense pressure builds up inside this confined space. This pressure is exerted directly onto the sensitive nerve endings, which is the direct cause of the throbbing, persistent, and often excruciating pain that signals a serious problem.
The Two Stages of Pulpitis: Reversible vs. Irreversible
Understanding your toothache is the first step towards finding lasting relief. It’s important to know that not all tooth pain from pulp inflammation is the same. The condition, known as pulpitis, falls into two distinct stages, which determine the urgency and type of treatment you need. Acting quickly at the first sign of trouble can make the difference between a simple filling and the need for more advanced care.
Endodontists, the Experts in saving teeth, use precise diagnostic criteria to determine the health of the pulp. The key distinction they make is between a pulp that is inflamed but can heal, and one that is damaged beyond repair. These two stages are known as Reversible vs. Irreversible Pulpitis, and identifying which one you have is critical for saving your tooth.
Reversible Pulpitis: A Warning Sign
Think of this stage as your tooth’s early warning system. The inflammation is mild, and the pulp is still healthy enough to recover if the source of irritation is removed. The pain is typically a sharp, sudden twinge that occurs in response to a trigger, like a cold drink or a sweet food. Crucially, the pain disappears within a few seconds of the trigger being removed. This is a clear sign that something is wrong, but with prompt and simple treatment-often just a dental filling to remove decay-your pulp can heal completely.
Irreversible Pulpitis: When the Pulp Cannot Heal
If the irritation continues, the inflammation can become so severe that the delicate pulp tissue cannot recover. This is irreversible pulpitis, a much more serious condition. The symptoms are very different: the pain is often a spontaneous, intense, and throbbing ache that lingers for minutes or even hours. It may be triggered by heat and can often feel worse when you lie down at night. At this stage, the pulp is in the process of dying, and you are facing a dental emergency. Urgent professional treatment, such as a root canal, is required to remove the damaged pulp, clean the tooth, and prevent the infection from spreading.
| Symptom | Reversible Pulpitis | Irreversible Pulpitis |
|---|---|---|
| Pain Type | Sharp, short-lived sensitivity | Dull, throbbing, intense ache |
| Pain Triggers | Mainly cold and sweet things | Often spontaneous, or triggered by heat |
| Pain Duration | Stops seconds after the trigger is gone | Lingers for minutes or hours; can be constant |
| Outcome | The pulp can heal with simple treatment | The pulp cannot heal; needs root canal treatment |
Pulp Necrosis: The Danger of Ignoring the Pain
It can be confusing when a severe toothache suddenly stops. While you might feel relieved, this often signals the final stage: pulp necrosis. This means the nerve tissue inside the tooth has died completely and can no longer send pain signals. However, the infection remains. Without treatment, this silent infection can spread beyond the root tip, forming a painful abscess in your jawbone. This is why it is vital to see a dentist even if the pain goes away on its own.
What Causes Pulpitis? From Decay to Dental Trauma
If you are struggling with the intense, persistent pain of an inflamed tooth, please know you are not alone. Pulpitis is an incredibly common dental condition, and understanding what causes it is the first step toward finding lasting relief. In every case, the core issue is the same: one of your tooth’s protective outer layers has been breached, allowing bacteria or severe irritation to reach the delicate, living pulp inside. This breach can happen in several ways, but they all require professional, compassionate care to resolve.
Deep Tooth Decay (Cavities)
The most common culprit behind pulpitis is, without a doubt, deep tooth decay. A cavity begins when bacteria in your mouth produce acids that erode the hard, protective enamel. If not treated, this decay progresses into the softer dentin layer beneath. Once it burrows deep enough to reach the pulp chamber, bacteria can invade the sterile environment, causing a direct infection. Your body’s response is to send blood cells to fight the infection, which causes swelling and pressure inside the rigid tooth, leading to the classic and often severe symptoms of pulpitis.
Trauma and Injury
A physical injury can also lead to pulp inflammation. A sudden impact from a fall or sporting accident can crack or fracture a tooth, creating an immediate and open pathway for bacteria to enter the pulp. However, trauma isn’t always a single, dramatic event. Chronic teeth grinding or clenching (bruxism) places immense, repetitive stress on your teeth, which can cause microscopic cracks to develop over time. Even if a crack is invisible to the naked eye, it can be wide enough to compromise the pulp’s seal and cause significant pain.
Previous Dental Work
Ironically, sometimes the very treatments designed to protect your tooth can contribute to pulpitis later on. A very deep filling, for example, places the restorative material extremely close to the pulp, and the heat and vibration from the procedure can sometimes lead to irritation. Furthermore, a tooth that has undergone multiple procedures-such as having an old filling replaced several times-experiences cumulative stress. This is a known risk and not necessarily a sign of poor dental work, but rather a reflection of the tooth’s complex history and the sensitivity of the nerve within.

Recognising the Symptoms: Is Your Toothache an Emergency?
We understand that any kind of tooth pain can be frightening, and it’s often difficult to know how serious it is. Is it something that can wait, or do you need to see a expert immediately? Differentiating between the stages of pulpitis is key to understanding what your tooth is telling you.
This guide is designed to help you recognise the specific signs, so you can feel empowered to get the right care at the right time. Use this checklist to assess your symptoms and determine your next steps.
Symptoms of Reversible Pulpitis (Act Soon)
This is the earliest stage, where the inflammation in your tooth’s pulp is still mild. The nerve is irritated but has the potential to heal if the cause is treated quickly, often with a simple filling. Don’t ignore these early warning signs.
- A sharp, quick pain when your tooth is exposed to something cold, sweet, or acidic.
- The discomfort disappears within a few seconds of the trigger being removed.
- The pain is not spontaneous; it only happens in response to a stimulus.
Symptoms of Irreversible Pulpitis (Act Urgently)
At this stage, the inflammation has become too severe for the pulp to heal on its own. The pain becomes more persistent and intense. Seeking urgent care from an endodontist is crucial to relieve the pain and save your tooth, usually with root canal treatment.
- A dull, throbbing ache that can be constant or intermittent.
- Intense, sharp pain that lingers for 30 seconds or longer after a trigger.
- Spontaneous pain that starts without any reason, even waking you up at night.
- Pain that worsens when you lie down due to increased pressure on the tooth.
- Lasting sensitivity to heat that continues long after the hot food or drink is gone.
Signs of a Spreading Infection (Emergency – Act Now!)
These symptoms are a clear signal that the infection has moved beyond the tooth’s pulp and into the surrounding bone and tissue. This is a serious dental emergency that requires immediate attention to prevent the infection from spreading further and causing significant health complications.
- Visible swelling in your gum, cheek, face, or jaw.
- A small, pimple-like bump (an abscess or fistula) on the gum near the painful tooth.
- A high temperature, fever, or feeling generally unwell and run-down.
If you have these signs, call us for an emergency appointment immediately. Your health is our priority, and we are here to provide swift, compassionate care.
How a expert Treats Pulpitis to Relieve Your Pain
Understanding the cause of your toothache is the first step, but finding a solution is what truly matters. When you’re in pain, you need a clear path to relief and the confidence that your tooth can be saved. At Root Canal London, our focus is on providing a calm, reassuring experience, led by a endodontist Endodontist-a dentist with advanced training in diagnosing and treating complex issues inside the tooth, including pulpitis.
The Diagnostic Process: Finding the Cause
Your journey to relief begins with a gentle and thorough examination to pinpoint the exact source of your pain. We listen carefully to your symptoms before conducting a few simple, painless tests. These may include:
- Pulp Vitality Tests: A cold stimulus is briefly applied to the tooth to check the nerve’s response. This is a quick and non-invasive way to understand the health of the pulp.
- Dental X-rays: These images allow us to see the tooth’s roots and surrounding bone, helping us identify deep decay, infection, or other underlying issues not visible to the naked eye.
This careful diagnostic process ensures we recommend the most effective and appropriate treatment for you.
Treating Reversible Pulpitis
If we catch the inflammation early, the treatment is often simple and highly effective. The goal is to remove the source of irritation-most commonly dental decay-and allow the pulp to heal on its own. This usually involves carefully cleaning out the decay and placing a dental filling or crown to protect the tooth. For patients with reversible pulpitis, this provides a swift and welcome end to their discomfort.
Saving Your Tooth: Root Canal for Irreversible Pulpitis
When the pulp is too damaged to heal, a root canal is the definitive solution to save your natural tooth and eliminate the infection for good. Far from the myths you may have heard, a modern root canal is a pain-relieving procedure. Under the care of a expert, the infected or inflamed pulp is gently removed, the inside of the tooth is meticulously cleaned and disinfected, and then sealed to prevent future problems.
This treatment stops the pain at its source and allows you to keep your own tooth, which is always the best option for your long-term oral health. To learn more about this comfortable, tooth-saving procedure, read our detailed guide: What is a Root Canal?
If tooth pain is disrupting your life, don’t wait. Contact our caring team today for a Endodontist assessment and find lasting relief.
Find Calm and Lasting Relief from Pulpitis
Understanding the source of your toothache is the first step toward finding relief. As we’ve explored, pulpitis is an inflammation of the dental pulp that can be either reversible or irreversible. The most important thing to remember is that prompt action is key-addressing the symptoms early can stop the pain, prevent infection, and ultimately save your natural tooth.
You don’t have to navigate this discomfort alone. At Root Canal London, our care is delivered by a expert Endodontist who uses advanced technology to provide effective, tooth-saving treatment. We are committed to ensuring you have a calm and reassuring patient experience, putting your comfort and well-being first at every stage.
In pain? Don’t wait for it to get worse. Book an appointment with our expert today.
Let us help you get back to a life free from dental pain.
Frequently Asked Questions About Pulpitis
Can pulpitis heal or go away on its own?
This depends on the stage. Reversible pulpitis, where the inflammation is mild, can heal if the cause (like a small cavity) is treated quickly by your dentist. However, irreversible pulpitis will not go away on its own. At this stage, the nerve tissue inside the tooth is too damaged to recover. Seeking professional, compassionate care is the only way to resolve the pain and save the tooth from further damage or infection.
How can I relieve pulpitis pain at home while I wait for my appointment?
While you await your appointment, you can manage the discomfort with over-the-counter painkillers like paracetamol or ibuprofen (always follow packet instructions). Applying a cold compress to your cheek for 15-minute intervals can also help reduce swelling. Try to avoid very hot, cold, or sugary foods that trigger sensitivity. These are temporary measures, and it is vital to see an endodontist for a permanent, pain-relieving solution.
Is pulpitis considered a dental emergency?
Yes, the severe, throbbing pain associated with acute or irreversible pulpitis is absolutely a dental emergency. This intense pain is a clear signal of significant inflammation or infection within your tooth that requires immediate attention. We understand how distressing this can be and offer same-day emergency appointments to provide a swift diagnosis and bring you calm, effective relief. Please do not hesitate to call us for urgent care.
What happens if I ignore irreversible pulpitis and don’t get a root canal?
Ignoring irreversible pulpitis can lead to serious complications. The infection will worsen, causing the nerve tissue to die (a condition called necrosis). This can lead to a painful abscess forming at the root of the tooth, which can damage the surrounding jawbone. In severe cases, the infection can spread to other parts of your body. Ultimately, the tooth will likely be lost. A root canal is a skilled procedure designed to prevent this, saving your natural tooth.
Will antibiotics cure pulpitis?
No, antibiotics alone cannot cure pulpitis. While they may be prescribed to manage a bacterial infection that has spread from the tooth into the surrounding gum or jaw (an abscess), they cannot reach the source of the problem. The inflamed or infected tissue is sealed inside the tooth. The only effective treatment is a dental procedure, like a root canal, to physically remove the damaged pulp and resolve the issue permanently.